Leading Through Ongoing Change: The Complexity of Leading in Healthcare Series Part 3 of 3
Denise Roistacher • February 6, 2026
Why Change Feels Hard—and How Leaders Can Help
In this series on the complexity of leading in healthcare, I’ve explored strategic thinking and psychological safety. This third focus—managing change—brings those threads together. Change is the context in which strategy is executed and psychological safety is either strengthened or eroded.
Managing Change in Healthcare
In healthcare, we often associate change with large, visible events: mergers, restructures, new systems, and new leadership. These moments are disruptive and disorienting, and they usually come with formal change plans, communications, and timelines.
Big change tends to challenge identity:
- Who am I in this new system?
- What is expected of me now?
It’s understandable that these moments trigger strong emotional reactions.
But some of the most taxing change in healthcare arrives quietly. Small shifts—new documentation requirements, workflow tweaks, additional metrics, policy updates—rarely get labeled as “change” at all. And yet, over time, they accumulate.
Each one subtly alters how work gets done, adds mental strain and chips away at a sense of predictability. Individually, these changes may seem manageable; collectively, they can be exhausting.
The Leader’s Role—Whether You Name It or Not
In times of change, leaders are in a role whether they claim it explicitly or not: to help people navigate what is shifting.
This doesn’t mean having all the answers or removing uncertainty. It means recognizing that people are constantly scanning for cues—often beginning with the most fundamental question:
- Is my job safe?
- Is this temporary?
- Am I supported?
Leaders’ words, tone, and behavior carry disproportionate weight.
This is true for major organizational change and for the small, day-to-day adjustments that rarely make the agenda. When leaders fail to acknowledge even minor changes, teams are left to interpret them on their own—often filling gaps with worry or assumptions.
When leaders slow down just enough to name what’s changing, what’s staying the same, and what people might reasonably feel, they provide stability and orientation. In healthcare environments where capacity is constrained and the work carries real consequences, that grounding matters.
How leaders show up shapes whether people feel engaged or adrift.
Why Both Trigger Real Emotional Reactions
Whether the change is large or small, people tend to ask the same unspoken questions:
- What does this mean for me?
- Will I still be competent?
- Will I have control or a voice?
- What am I losing—even if no one is naming it?
In healthcare, where capacity to focus is already stretched and the consequences matter deeply, even “small” changes can tip people into:
- Irritability or resistance
- Withdrawal or disengagement
- Over-functioning (“I’ll just do more to stay ahead”)
- Cynicism (“This too shall pass…”)
One helpful way to understand these reactions is through the change curve, often associated with the Kübler-Ross model. While originally developed to describe grief, it has been widely applied to organizational change because it captures a universal experience: when familiar ways of working are disrupted, people move through recognizable emotional responses.
Shock or denial may show up as disbelief or minimization. Frustration and anger often emerge as resistance. Low energy or confusion can follow, before experimentation, acceptance, and renewed engagement begin to take hold. Importantly, people do not move through this curve neatly or at the same pace—and they may revisit stages as new changes continue to layer on.
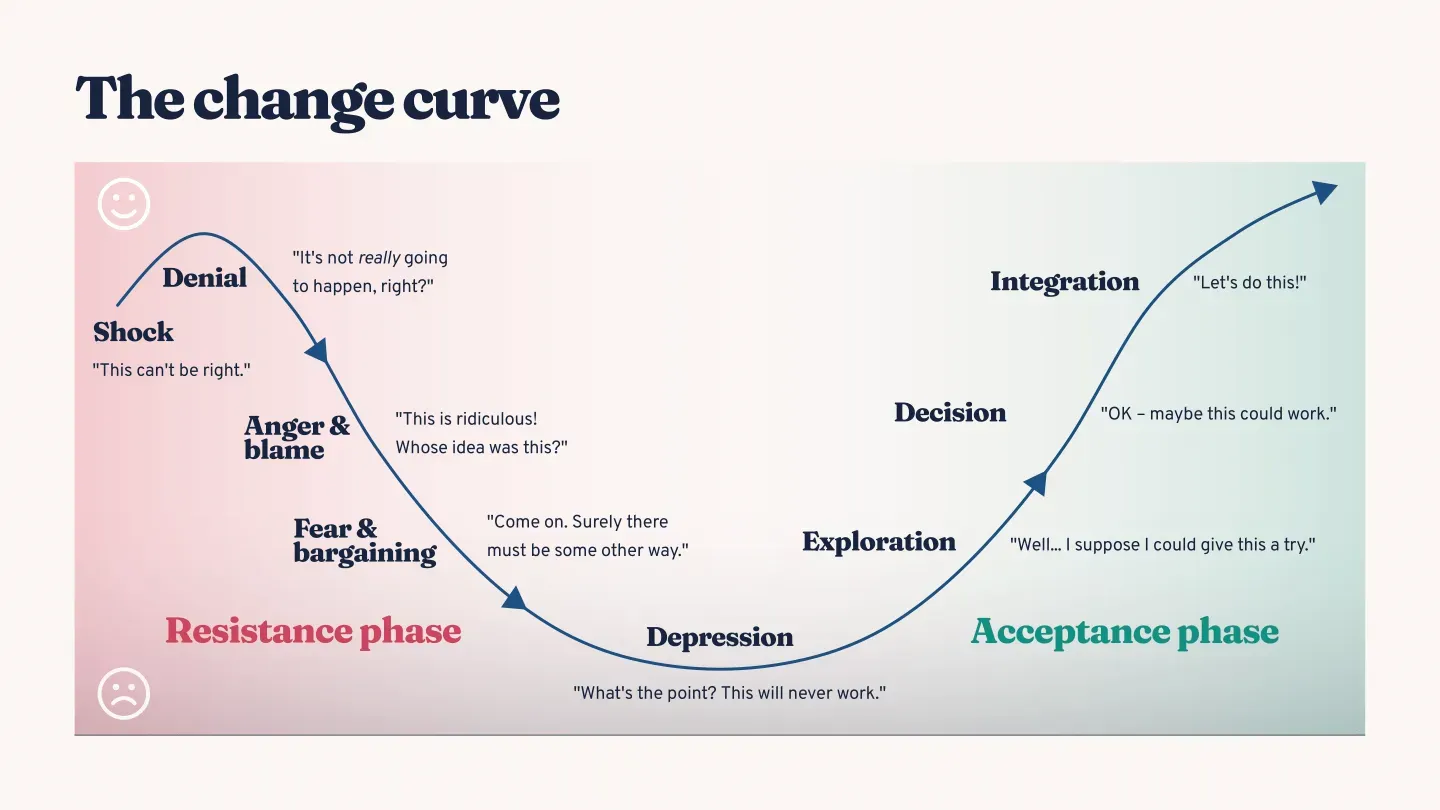
A simplified view of the emotional change curve. (above)
You may recognize yourself—or notice different members of your team—at different points on this curve at the same time.
Many teams experience change in much the same way—disoriented, unsure of the rules, and quietly wondering how to regain their footing. The leader’s role isn’t to rush people down the change, but to help them make sense of where they are on the journey and remind them they’re not walking it alone.
The nervous system doesn’t distinguish between strategic and administrative change—it simply registers loss of familiarity and increased demand. Big change disrupts identity. Small change disrupts rhythm. Both matter.
Managing Resistance
Resistance isn’t just pushback—it’s valuable data about how change is landing with your team. Instead of viewing resistance as something to eliminate, approach it with curiosity.
Ask yourself:
- What is this telling me about how people are experiencing this change?
Think of resistance as a signal pointing to concerns, unmet needs, or barriers you may not yet see. When leaders respond with patience rather than judgment, resistance becomes an opening rather than an obstacle.
Curiosity builds connection. Listening builds trust. Over time, this stance allows leaders to engage more authentically with their teams—even when the change itself remains hard.
Leadership in Collective Disruption
When change is profound and collective, such as during a pandemic, a national tragedy, or a disruption that affects the entire organization, individual sense-making is not enough.
People need space to process together.
In these moments, leaders can bring the community into shared reflection through intentional forums: listening sessions, thoughtfully designed town halls, or facilitated conversations that allow people to name what they experienced.
These gatherings are not about solving problems or driving alignment; they are about helping people absorb the emotional and psychological impact of what they have lived through. When done well, these shared conversations reduce isolation, support collective resilience, and help teams move through trauma rather than carrying it silently into the next phase of work.
Creating space for shared reflection does not replace action. It prepares people for it.
Practical Steps Leaders Can Take
Once leaders understand the emotional terrain of change, the work becomes less about tactics and more about guidance and support.
Communication:
Use a variety of communication venues. Don’t rely solely on email or posted memos—bring up changes in
- one-on-one meetings,
- daily huddles,
- open office hours scheduled on Outlook/Teams
- staff meetings, and
- town halls.
Each format creates a different opportunity: 1:1s allow private concerns to surface; huddles create quick alignment; staff meetings build shared understanding; town halls address broader questions and reinforce transparency.
A few consistent actions can make a meaningful difference:
Name the change—early and often.
Even small shifts deserve acknowledgment.
- “This is another change, and I want to acknowledge the adjustment it asks of you.”
- “I know this wasn’t something anyone asked for, and I appreciate the flexibility it requires.”
- “Even small updates take energy to absorb—thank you for adapting while keeping the work moving.”
Naming change in this way doesn’t slow momentum; it strengthens it. People are more willing to lean in when they feel their reality has been recognized.
Differentiate what’s changing from what’s staying stable.
- Naming constants—priorities, values, routines—helps regulate anxiety. Note what is staying the same.
Explain the ‘why,’ even briefly.
- People don’t need certainty, but they do need to understand the rationale for the change. .
Invite input without over-promising.
- Ask where the change is creating friction and be honest about what is and isn’t adjustable.
Close the loop.
- Reflect back what you’re hearing across the team. Even when immediate action isn’t possible, acknowledgment builds trust.
Practice active listening.
Go beyond sharing information—listen for concerns, questions, and emotion.
- Paraphrase: “What I’m hearing is that this feels overwhelming right now.”
- Clarify: “Can you say more about what feels unclear?”
- Validate: “It makes sense you’d feel frustrated by another requirement.”
- Summarize: “The process works, but the timing is challenging.”
These responses help people feel heard and open the door to more honest dialogue.
These steps won’t remove discomfort, but they prevent unnecessary strain from going unnamed—and help teams stay grounded while navigating ongoing change.
Final note:
Emotional intelligence is also critical during periods of change. This includes attending not only to your team’s emotions, but to your own. Notice your reactions—frustration, reluctance, worry—and model healthy responses. Demonstrating self-awareness, adaptability, and openness to feedback sets the emotional tone for the system.
Change is constant in healthcare. How you show up as a leader makes a tangible difference.
What is one step you will take this week to support your team through change?
Series Wrap-Up
As this series comes to a close, a clear throughline emerges: effective healthcare leadership is less about having the right answers and more about creating the conditions for people to think, speak, and adapt together. Strategic thinking provides direction. Psychological safety allows people to raise concerns, ask questions, and learn from mistakes without fear. Managing change is where both are tested—day by day, decision by decision.
When leaders attend to the human experience of change, they don’t just help teams move through transitions; they help them stay connected, capable, and engaged in work that truly matters.











